In India, spice isn’t just a flavor, it’s a way of life — from rich curries to kicking chutneys, the heat is part of the experience. But sometimes, what starts as a fiery flavour can end in sharp abdominal pain, burning throat, and a feeling that something isn’t right.
Across the globe, digestive-tract disorders related to food are rising, with up to 20–25% of adults reporting regular digestive symptoms. In Asian countries where spicy food is more common, research shows effects of capsaicin (the compound that gives chillies their heat) on the gut can lead to discomfort and pain.
Dr. Shashank Agrawal, a distinguished Gastrointestinal Surgeon in Ghaziabad, explains:
“When someone eats something with strong spice and then feels severe abdominal pain, it’s not simply the spice doing its job. What we often see is that the stomach lining, or the oesophagus, has become sensitive — sometimes due to repeated acid exposure, sometimes due to inflammation. My goal is to identify what’s causing that pain, treat it safely, and help the patient return to meals they enjoy without fear.”
Thinking the heat is just ‘normal digestive trouble’? Let’s explore what that pain might actually mean.
Causes of Abdominal Pain after Eating Spicy Food
In many cases, a mild burning sensation after spicy food is harmless. But when the pain is intense, lasts longer than expected, or comes with other symptoms, it could indicate an underlying problem. Some of the common reasons include:
Increased acid secretion: Spicy foods can stimulate acid production, which may irritate the stomach or oesophagus.
Gastritis (inflammation of the stomach lining): Repeated irritation from spicy food or acid can inflame the stomach lining, leading to sharp pains, nausea or a feeling of fullness.
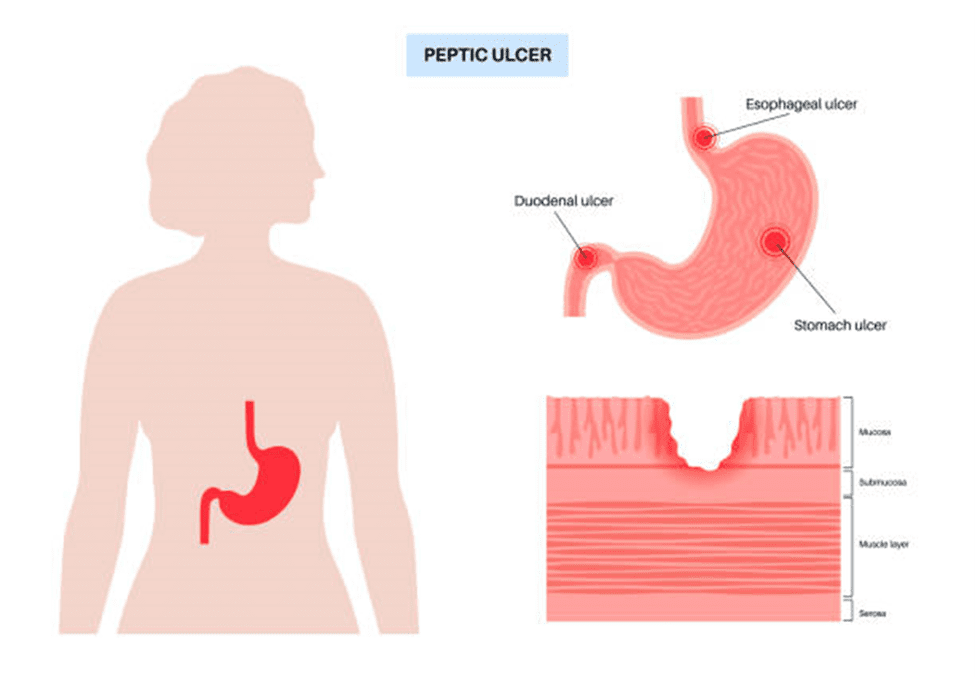
Peptic ulcers: Though ulcers have many causes (such as H. pylori infection), frequent exposure to acid combined with irritants like spicy food may worsen the condition.
Functional dyspepsia / sensitive gut: Some people have an increased sensitivity in their digestive tract; spice may trigger pain even in the absence of visible damage.
Acid reflux / gastro-oesophageal reflux disease (GERD): Spicy meals can loosen the lower oesophageal sphincter, allowing acid to come up and cause burning pain.
Irritable bowel syndrome (IBS) triggers: Research shows individuals consuming very high amounts of spice may have a higher chance of IBS-related pain.
Could your love for spice be quietly triggering something deeper? Let’s find out.
How Spicy Food Can Trigger Acid Reflux, Gastritis, and Ulcers
- Spicy foods may irritate the stomach lining, especially if it’s already inflamed.
- Acid reflux is more likely when the lower oesophageal sphincter is weakened, and strong meals (including hot spices) can prompt reflux episodes.
- In cases where someone already has gastritis or an ulcer, eating spicy food may cause sharper pain, bleeding, or complications.
- For individuals with heightened gut sensitivity, chili and similar foods can amplify the pain response.
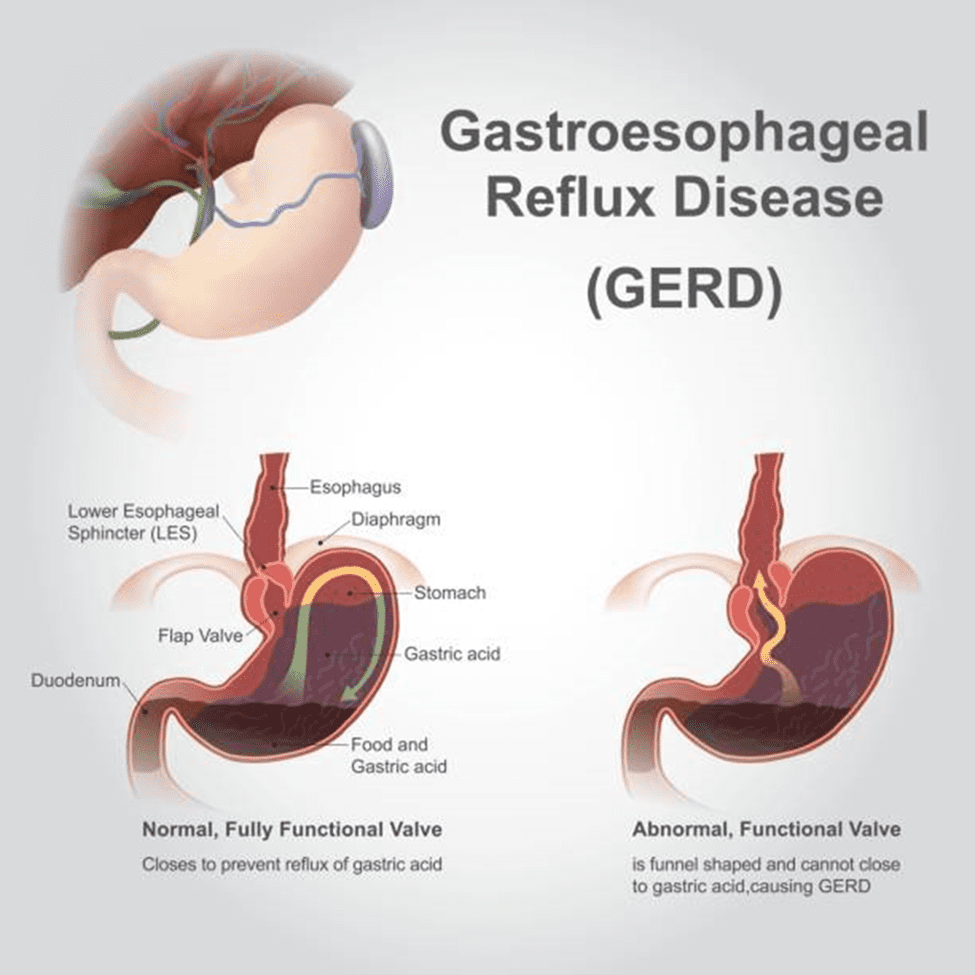
Dr. Shashank Agrawal, a trusted expert for Acid Reflux / GERD Treatment in Ghaziabad, says:
“We often tell patients that spice isn’t inherently bad — it’s how the body responds that matters. If the lining of your stomach or oesophagus has been battered by acid or inflammation before, then eating a highly spicy meal may set off pain. The trick is to understand your own trigger threshold, find out if there’s lasting damage, and tailor treatment so you can still enjoy flavour, safely.”
Do not ignore your gut health—consult a gastroenterologist today.
Looking for practical ways to ease that pain tonight? Here’s what you can do.
Ways to Relieve Abdominal Pain and Prevent Discomfort after Spicy Meals

Here are helpful steps that many find useful:
- Try cutting back the quantity of chillies or opting for milder blends.
- Eat smaller meals as large, heavy, spicy meals make the stomach work harder and increase acid risk.
- Give yourself at least 1-2 hours after eating before lying down; elevate your upper body if needed.
- Include soothing foods, bland foods like rice, curd, oats or bananas may reduce irritation.
- Stay hydrated, water helps dilute acid and supports digestion.
- If you find that certain spices (like red chillies, black pepper, or garlic) consistently cause pain, limit them.
- Use over-the-counter relief cautiously, antacids or acid-reducing medications may help short-term but if pain is frequent, you’ll want a lasting solution.
But when should that discomfort trigger a full-fledged consultation? Let’s check the red flags.
Recognizing When Persistent Abdominal Pain Requires Medical Attention
Frequent, severe pain after spicy food needs careful attention. It is time to see a gastroenterology doctor when:
- The pain lasts more than a day or recurs regularly after meals.
- You experience additional symptoms like vomiting, weight loss, blood in stool, dark stools, or difficulty swallowing.
- You have known risk factors such as a prior history of ulcers, acid reflux, or heavy alcohol/smoking history.
- You find that spicy food triggers more than just a mild burn — for instance, sharp pain, chest discomfort, or pain radiating to the back.
- You’ve used acid-suppressing medications or antacids for weeks without relief.
Dr. Shashank Agrawal, among the leading GI surgeons in Ghaziabad, notes:
“My red-flag checklist is simple: persistent pain, signs of bleeding or weight loss, any alarm symptom around swallowing or chest pain. If any of these apply after a spicy meal, don’t wait. Early testing (endoscopy, pH monitoring) can catch early damage, prevent complications and let you get back to normal food with confidence.”
Let’s wrap this up with a quick overview of what you’ve learned and why it matters.
Conclusion
Enjoying spicy food is part of our culture and our pleasure. But if after every hot meal you’re met with severe abdominal pain, burning sensation or acid-like symptoms, it’s more than just “too much spice.” It might signal underlying issues such as reflux, gastritis or even early ulceration.
Recognising the pattern is half the battle …
Changing habits, checking triggers, and when needed, seeking specialised care can make all the difference.
Curious what questions others often ask? Here are five that might match yours.
FAQ
Q1: Can I still eat spicy food if I have acid-reflux or gastritis?
Yes — in many cases you can. The key is moderation, identifying your personal tolerance, and pairing spice with protective habits (smaller meals, avoid lying down, include dairy or rice to buffer spice). But if symptoms persist, speak with a specialist.
Q2: Does spicy food alone cause ulcers?
Spicy food by itself usually doesn’t cause ulcers. Common causes of ulcers include infection with H. pylori, long-term NSAID use and heavy acid exposure. But spice can aggravate an existing ulcer or make symptoms worse.
Q3: Is a burning sensation after eating spicy food always serious?
Occasional mild burning might just mean your stomach is sensitive. But if you get repeated pain, difficulty swallowing, vomiting, or black stools, that suggests a more serious issue and you should see a doctor.
Q4: How long does it take for stomach lining to heal if it’s irritated by spicy food?
Mild irritation may improve in a week with diet changes and medications. If there’s erosion or inflammation (gastritis), healing might take a few weeks to months and requires follow-up.
Q5: Will antacids prevent the pain from spicy food?
Antacids can help reduce acid and provide short-term relief, but they don’t fix underlying causes like reflux, weakened oesophageal sphincter or gastritis. If you find you rely on antacids often, it’s time to see a GI surgeon.
References
https://www.mayoclinic.org/diseases-conditions/gerd/symptoms-causes/syc-20361940
Disclaimer: The information shared in this content is for educational purposes only and not for promotional use.


Hi, this is a comment.
To get started with moderating, editing, and deleting comments, please visit the Comments screen in the dashboard.
Commenter avatars come from Gravatar.