For many people, the question of how long they will be out of action is often one of the first when they are told they need abdominal surgery. Recovery today, with modern surgical techniques and specifically advanced minimally invasive surgery, stands in contrast to what has been considered ‘recovery’ in the past. With laparoscopic surgery, you will enjoy a faster recovery after the surgery because it involves small incisions that cause less surgical trauma, consequently allowing you to return to daily activities in a week or two, rather than the four to six weeks generally associated with open surgeries.
But what does it mean? At our clinic, we have seen that minimally invasive surgery may translate into less post-operative pain and easier post-operative recovery. And as one of the accomplished laparoscopic surgeons in Ghaziabad, we’re well aware that your option of surgical approach indeed shapes your road to recovery. The dissimilarities between laparoscopic vs open surgery recovery aren’t just in scar sizes; they influence infection risk, pain, hospital stay, and quick return to normal life.
This article digs into a number of reasons why advanced laparoscopic surgery brings about improved post-surgical outcomes. If you are thinking about gallbladder removal, hernia repair, or any other gastrointestinal procedure with a gastroenterologist in ghaziabad, it is necessary to highlight these important benefits that allow you to reach a final decision. The concentration of Dr. Shashank Agrawal lies in advanced techniques of laparoscopy, reducing surgical trauma and therefore promoting safe surgical recovery.
What Is Early Dumping Syndrome and What Does It Feel Like?
Early dumping syndrome occurs when food, particularly high-sugar or high-carbohydrate food, moves too rapidly from the stomach remnant into the small intestine, typically within 10 to 30 minutes of eating.
Rapid fluid shifts
When a large volume of osmotically active food enters the small bowel all at once, the body draws fluid from the bloodstream into the gut, causing a sudden drop in circulating blood volume.
Hormonal response
This rapid entry also triggers the release of gut hormones like serotonin and GLP-1, which further accelerate intestinal activity and cause vasodilation.
What patients experience
The resulting symptoms can feel alarming – nausea, abdominal bloating and cramping, explosive diarrhoea, heart palpitations, dizziness, hot flushes, cold sweats, and a sudden need to lie down. Many patients describe feeling as though they have lost all energy within minutes of finishing a meal.
It is important to note that early dumping syndrome is distinct from late dumping syndrome, which occurs 1–3 hours after eating and is caused by reactive low blood sugar. Both can occur in the same patient, but they require different management strategies.
Wondering why your surgery specifically raised this risk? Here’s the anatomy behind it.
Why Stomach Cancer Surgery Triggers This Condition
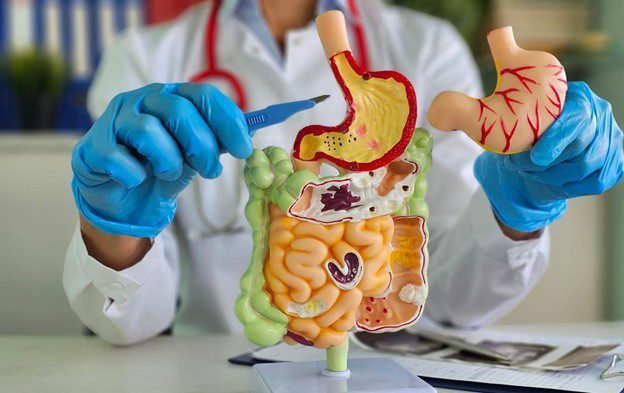
The type of gastrectomy performed, and the reconstruction technique used, directly determines how likely and how severe dumping syndrome will be –
Total vs. subtotal gastrectomy
Total gastrectomy carries the highest risk of dumping syndrome. Subtotal gastrectomy may result in milder symptoms but does not eliminate the risk entirely.
Loss of the pyloric valve
Most gastrectomy procedures bypass or remove the pylorus, the valve that controls how slowly food exits the stomach. Without it, there is no brake on gastric emptying.
Vagal nerve disruption
Surgery can disrupt the vagus nerve, which regulates gut motility. This can further accelerate how quickly food moves through the digestive tract, making dumping syndrome more pronounced.
Other factors that influence severity include the patient’s age, pre-operative nutritional status, and the presence of conditions like diabetes, which can affect how the body responds to rapid changes in blood sugar and gut hormone release.
Don’t let post-surgery symptoms go unaddressed. Consult Dr. Shashank Agrawal for expert stomach cancer recovery care today.
Dietary and Lifestyle Changes That Genuinely Help
Small, frequent meals
Eat 5 to 6 small meals a day to reduce the volume of food entering the intestine at one time.
Separate solids from liquids
Drink fluids 30 to 45 minutes after meals to prevent rapid gut transit.
Avoid simple sugars
Replace refined carbohydrates with complex carbs, lean proteins, and healthy fats for a slower digestive response.
Rest after meals
Lie down for 20 to 30 minutes post-meal to use gravity in slowing gut transit.
Increase dietary fibre:
Soluble fibre and thickening agents slow stomach emptying and reduce osmotic load on the small bowel.
Not getting enough relief from diet changes alone? Here’s when and how medicine steps in.
Medical Treatment and When to Seek Specialist Support
When dietary changes do not adequately control symptoms, medical management becomes the next step, and it is important not to delay seeking help.
Octreotide
This somatostatin analogue is one of the most well-evidenced treatments for dumping syndrome. Administered as a subcutaneous injection before meals, it slows intestinal motility, suppresses gut hormone release, and moderates fluid shifts. It is particularly useful for patients with moderate to severe symptoms.
Acarbose
This medication slows carbohydrate digestion and is sometimes added specifically when late dumping syndrome with reactive hypoglycaemia is present alongside early dumping.
Nutritional supplementation
Gastrectomy patients are at significant risk of deficiencies in iron, vitamin B12, calcium, and vitamin D. These must be monitored and supplemented regularly as part of ongoing post-operative care.
Surgical revision
In rare cases where both dietary and pharmacological management fail to provide relief, surgical revision of the reconstruction may be considered. This is only pursued after all conservative options have been thoroughly explored.
Dr. Shashank Agrawal notes:
“Patients sometimes wait months before mentioning dumping symptoms at a follow-up because they assume it’s normal. It is common — but it is not something you simply live with. There are very effective ways to manage it, and the sooner we address it, the better the nutritional and quality of life outcomes for the patient.”
Conclusion
Early dumping syndrome after stomach cancer surgery is a recognised, manageable, and often reversible complication — but only when it is identified and addressed properly. The absence of the stomach’s normal regulatory function after gastrectomy creates a new digestive reality for patients, one that requires structured dietary adaptation, regular specialist follow-up, and, where needed, medical support. Ignoring persistent post-meal symptoms or assuming they are an unavoidable part of recovery can lead to significant weight loss, nutritional deficiencies, and a diminished quality of life. With the right guidance and a consistent approach, most patients can regain control of their meals, their nutrition, and their day-to-day comfort after stomach cancer surgery.
Frequently Asked Questions
How soon after stomach cancer surgery does early dumping syndrome start?
Symptoms can begin within days to weeks of surgery, often as patients transition from a liquid to a soft and then solid diet. Early identification allows for prompt dietary adjustment before symptoms become established.
Is early dumping syndrome permanent after gastrectomy?
Not necessarily. In many patients, symptoms improve significantly within 6 to 12 months as the body adapts to its new digestive anatomy. With consistent dietary management, a large proportion of patients achieve substantial symptom control over time.
Can I eat normally again after being diagnosed with dumping syndrome?
Most patients return to a broad, enjoyable diet over time — with some modifications. The key is understanding personal triggers, meal size, and the timing of fluids. A dietitian working alongside your surgical team can help tailor a plan that fits your lifestyle.
What is the difference between early and late dumping syndrome?
Early dumping occurs within 10 to 30 minutes of eating and is driven by fluid shifts and gut hormone release. Late dumping occurs 1 to 3 hours after eating and is caused by reactive hypoglycaemia — a blood sugar crash triggered by insulin overproduction. Both can occur in the same patient.
When should I consult a doctor about my post-surgery symptoms?
You should seek specialist review if symptoms are occurring regularly, affecting your ability to eat or maintain weight, causing dizziness or fainting, or if you are losing weight without intending to. Early follow-up with a GI surgeon prevents complications and accelerates recovery.

